RADIOLOGY TESTING
ANCILLARY SERVICES PROVIDED AT CARDIOLOGISTS OF LUBBOCK
Stress Testing
A stress test, also called a cardiac stress test, shows how exercise affects your heart. A stress test determines how much exercise your heart can tolerate before having a problem. Doctors use stress tests to diagnose and monitor coronary artery disease, cardiac ischemia (not enough blood flow to the heart muscle), cardiac arrhythmias (abnormal heartbeats), and other types of heart disease. A stress test is only one method to monitor and diagnose heart conditions. There are several types of stress tests which can be performed and your doctor will schedule you according to what they feel is best for you. There are some physical and medication limitations which your doctor takes into consideration when ordering your stress test.
The types of stress tests include:
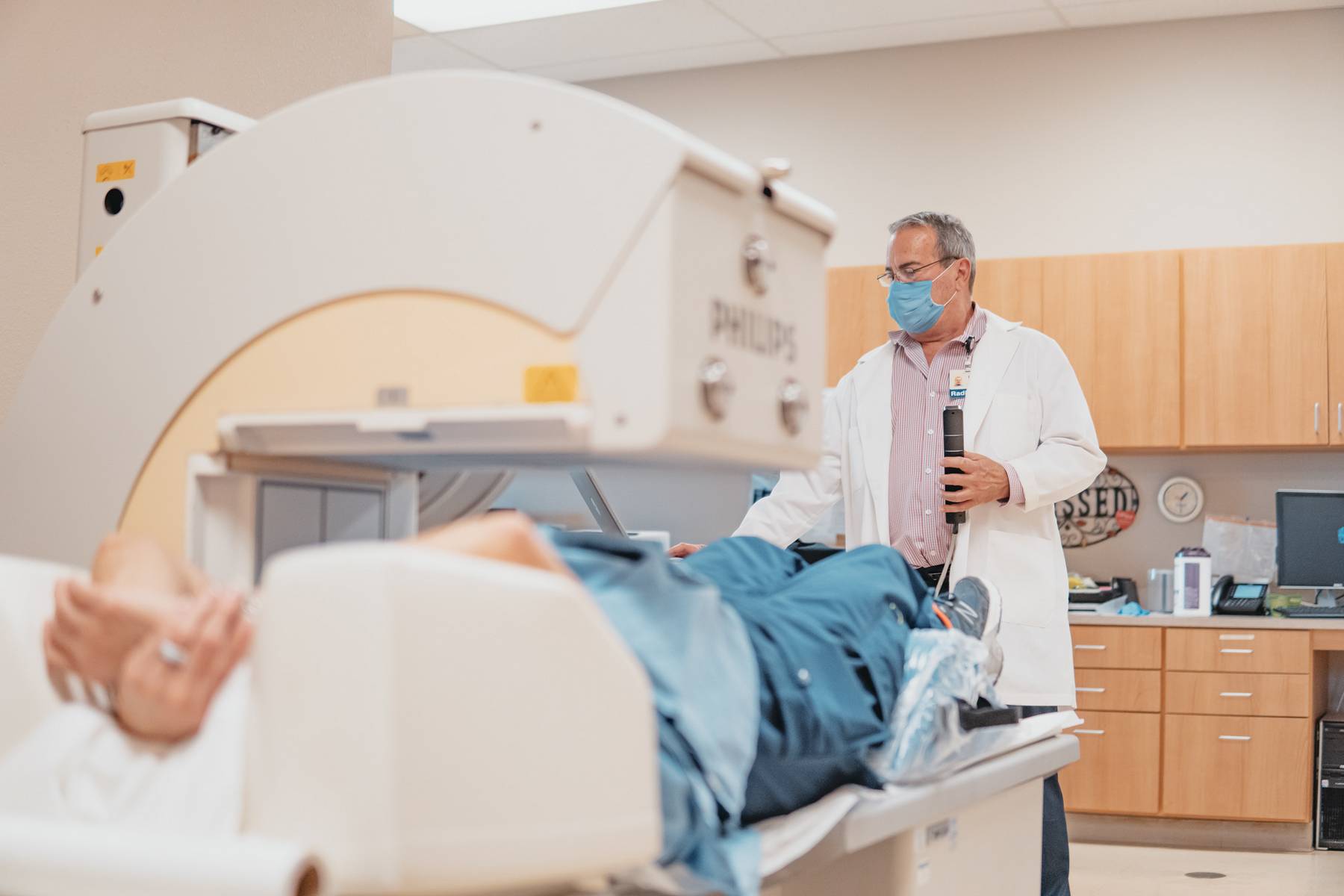
STANDARD OR REGULAR STRESS TEST
Also called an exercise stress test or treadmill test, involves walking on a treadmill while your ECG and blood pressure are being monitored. The test becomes harder (higher and faster) the longer you are able to exercise and until your specific maximum predicted heart rate is achieved.
HOLTER MONITOR
A Holter monitor is a type of heart monitor that records your heart’s activity over 24 or 48 hours. If you have an irregular heartbeat or heart palpitations, but an EKG didn’t detect anything, a cardiac monitor can help diagnose the problem. You wear the Holter monitor while you do your daily activities. Your provider discusses the results with you.
A Holter monitor can find the cause of:
– Arrhythmia (heart rhythm abnormalities).
– Heart palpitations.
– Unexplained dizziness.
Your provider can also use a cardiac monitor to determine how well your:
– Heart is getting oxygen.
– Heart medications are working.
– Pacemaker is working.
NUCLEAR STRESS TEST
This test is similar to the standard stress test but also involves using a radioactive tracer which allows the technologists to take pictures of blood flow to your heart muscle before and after the stress test. An IV will be required prior to the start of this exam to allow for administration of the radioactive tracer. This tracer does not cause any side affects but allows for imaging of your heart before and after the stress test.
CHEMICAL STRESS TEST (LEXISCAN, most commonly used in this facility)
This is a type of nuclear scanning test. It shows how well blood flows to the heart muscle. This nuclear stress test involves injecting a medication called Lexiscan into your IV while you are closely monitored. This medication takes the place of using a treadmill or other means of exercise. This test is used for people that are unable to exercise or can’t exercise for very long in order to reach predicted maiximal heart rate.
The lexiscan injection may cause a warm, flushing feeling. It is normal for your breathing rate, heart rate, blood pressure, and perspiration to increase during the test. If you begin to notice chest discomfort or pain, headache, upset stomach, dizziness or other symptoms of concern such as excessive shortness of breath, please let the stress lab personnel know. The above symptoms may be normal and typically go away within 3-4 minutes.
** Do not drink or eat foods containing CAFFEINE for 12 hours prior to your test. Products labeled decaffeinated and caffeine-free contain trace amounts of caffeine and should also be avoided. Caffeine will interfere with the results of your test. If you have had caffeinated products within 12 hours of your test, you will be rescheduled.
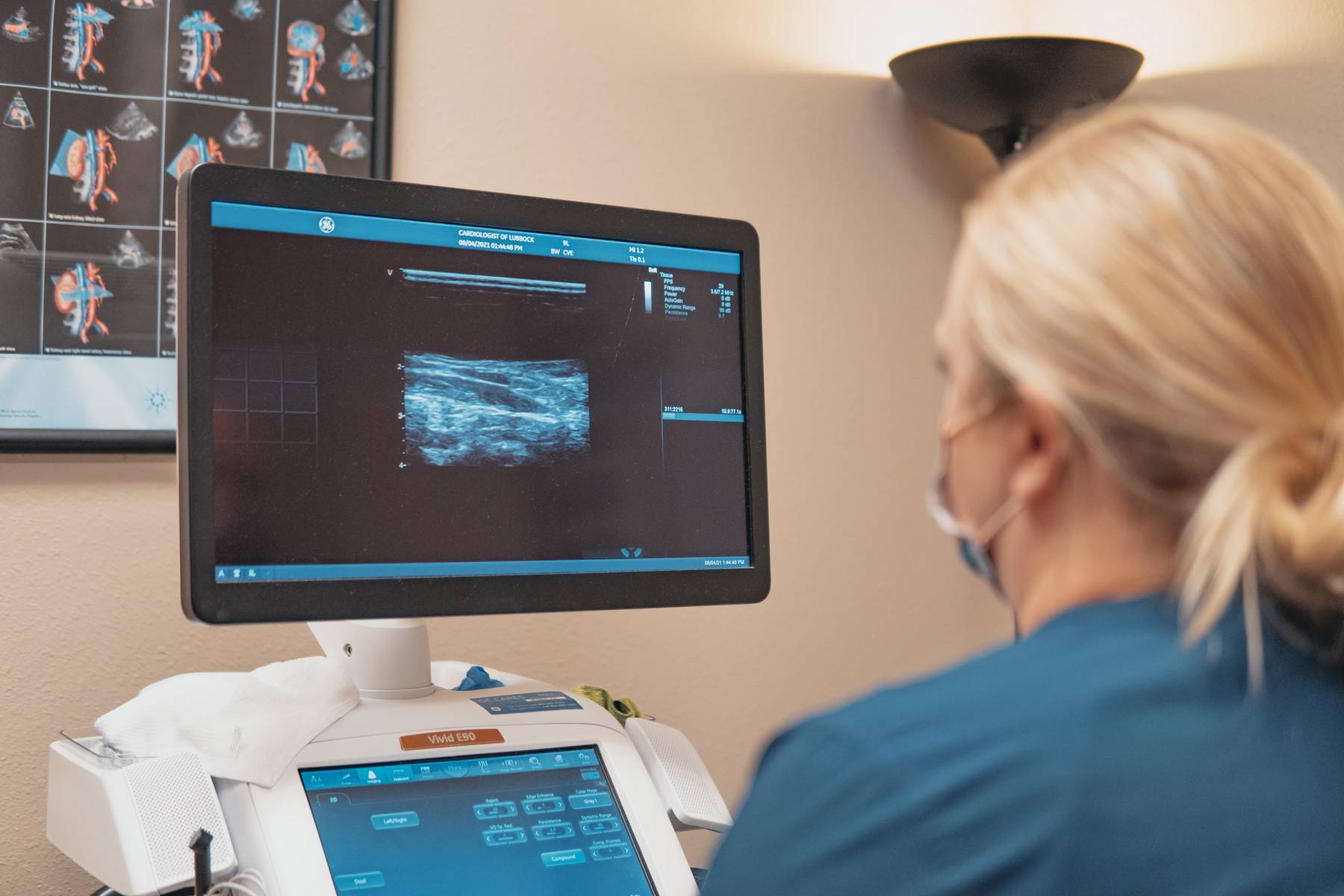
Peripheral Vascular Testing
Similar to an echocardiogram, peripheral vascular testing uses sound waves to produce images of the arteries or veins of your body. This allows your doctor to see blood flow in vessels and also to evaluate for blockage which can be caused by plaque build-up (arteries) or clots (veins). Following are peripheral vascular exams performed here in the office.
CAROTID DOPPLER (ultrasound)
Carotid ultrasound is a safe, painless, and non-invasive procedure that uses sound waves to examine the blood flow through the carotid arteries. Your two carotid arteries are located on each side of your neck. They deliver blood from your heart to your brain. Carotid ultrasound tests for blocked or narrowed carotid arteries, which can increase the risk of stroke. The results can help your doctor determine a treatment to lower your stroke risk.
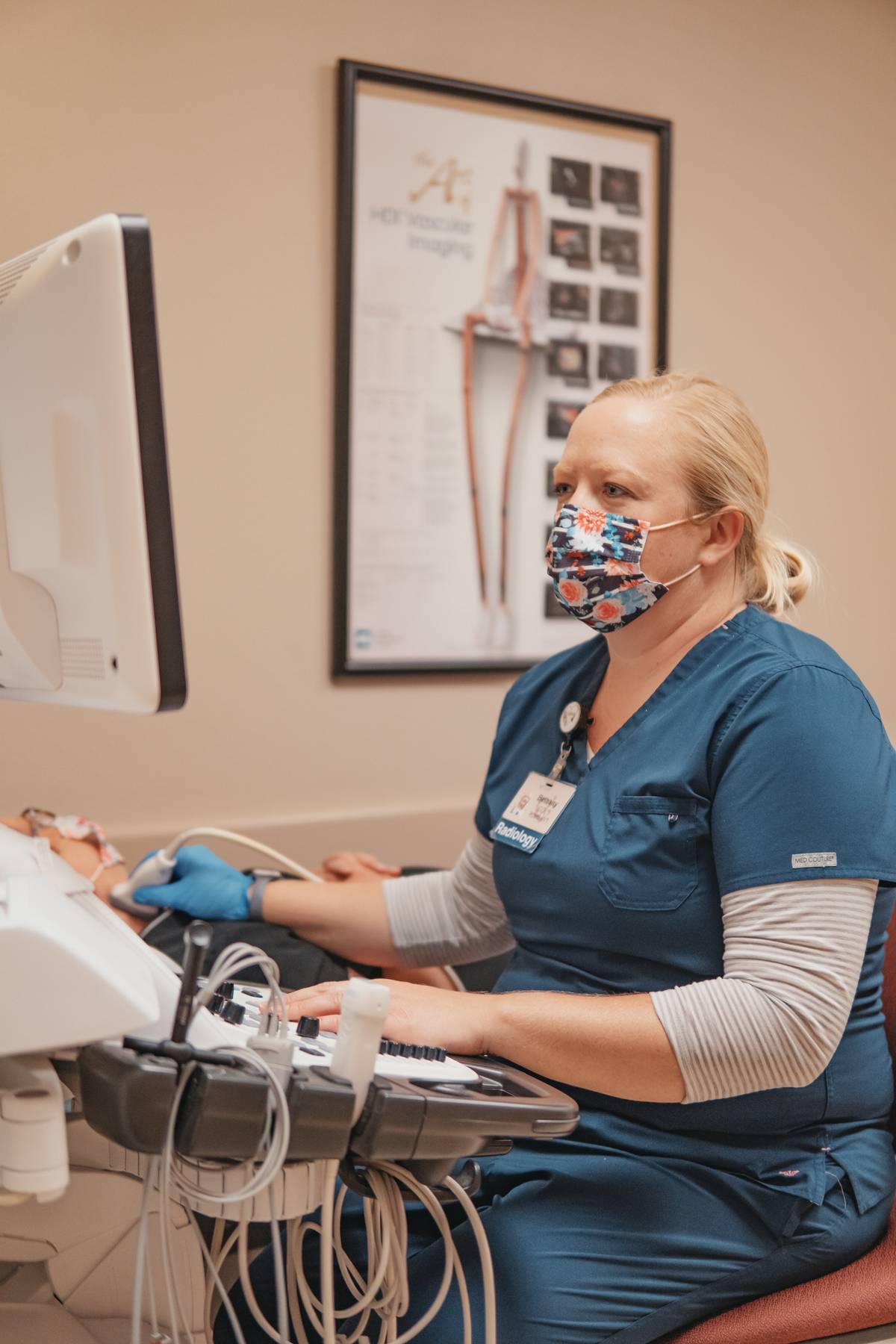
ARTERIAL DOPPLER (ultrasound)
Arterial doppler ultrasound is a noninvasive test that can be used to estimate the blood flow through your blood vessels in the legs and arms by bouncing high-frequency sound waves (ultrasound) off circulating red blood cells. During a doppler ultrasound, a technician trained in ultrasound imaging (sonographer) presses a small hand-held device, about the size of a bar of soap, against your skin over the area of your body being examined, moving from one area to another as necessary. Pressures may be evaluated at the beginning of this exam on your arms and legs. This is done to calculate an ABI, ankle brachial index. An arterial doppler ultrasound may help diagnose many conditions, including:
– A blocked artery (arterial occlusion)
– Decreased blood circulation into your legs (peripheral artery disease)
– Bulging arteries (aneurysms)
– Narrowing of an artery (stenosis)
– Blood clots
This test may be done as an alternative to more-invasive procedures, such as angiography, which involves injecting dye into the blood vessels so that they show up clearly on X-ray images. An arterial doppler ultrasound test may also help your doctor check for injuries to your arteries or to monitor certain treatments to the arteries.
VENOUS DOPPLER (ultrasound)
A venous doppler ultrasound is a diagnostic test used to check the circulation in the large veins in the legs or sometimes the arms. This exam shows any blockage in the veins by a blood clot or “thrombus” formation. Superficial thrombophlebitis (sometimes called phlebitis) is a clot that has formed in the veins near the surface of your skin. Clotting can occur after injury or in old varicose veins. Superficial thrombophlebitis usually responds very well to local treatment.
Deep Vein Thrombosis (sometimes called DVT) is a blood clot in a deep vein, resulting in partial or complete blockage of blood flow in that vein. The symptoms of this deep vein thrombosis can be vague. Pain, swelling and redness are usually found.
Unlike superficial thrombophlebitis, a DVT is a serious health concern, because it’s possible that the clot could break off and travel to your lungs. It is then referred to as a pulmonary embolism. The risk of pulmonary embolism is decreased if you recognize the symptoms of a DVT quickly and get it treated right away.
No one understands completely why some people are more likely than others to develop a DVT. Some situations increase the chance of clots forming in the deep veins:
– Surgery or injury
– Long-term bed rest or immobility
– Pregnancy
– Obesity
– A history of venous thrombosis
VENOUS INSUFFICIENCY DOPPLER (ultrasound)
A venous insufficiency ultrasound is done similar to the normal venous doppler of the legs but is specifically used to diagnose reflux in the veins. Venous reflux occurs when there is impaired return of blood from the veins in the legs and feet. This can cause symptoms such as swollen legs, varicose veins, skin breakdown, or ulcers.
How it is done: You will be asked to lie on your back. The exam table may be tilted with you head higher than your legs, and you may be asked to stand for a portion of the exam. Gel will be applied to each of your legs, and an ultrasound transducer (a small, hand-held wand) will be rubbed on your skin in order to obtain images of your blood vessels. You may be asked to change positions in order to obtain images of each vein. The technician will press the transducer on your legs and will squeeze your legs. This may cause a slight discomfort for some patients. A venous insufficiency ultrasound may take 30-45 minutes to complete.
RENAL ARTERY DOPPLER (ultrasound)
This type of doppler ultrasound is a test that uses sound waves to produce images of the body, specifically the kidneys in this case. If your doctor suspects you have renal artery stenosis, he or she may order a doppler ultrasound to view blood flow in the renal arteries. The test allows doctors to assess plaque buildup and identify narrowing of the arteries. Your physician may suspect renal artery stenosis if you have high blood pressure, especially if it is difficult to control. This can occur from narrowing of one or both renal arteries, the blood vessels that lead to the kidneys. This narrowing (stenosis) can develop as a result of atherosclerosis, plaque building up in the arteries. Fibromuscular dysplasia, a condition in which many arteries in the body are prone to narrowing, may also cause renal artery stenosis.
During the ultrasound, a technician places a hand-held instrument called a transducer against the abdomen. This device transmits sound waves that produce images of blood vessels and the flow of blood through them. The ultrasound can take 20 to 30 minutes to complete.
MESENTERIC ARTERY DOPPLER
A mesenteric artery ultrasound evaluates the arteries that supply blood to the intestines. Images are acquired using a hand held probe (transducer) that is applied to the abdomen.
This test is used to look for blockages or narrowing of the mesenteric arteries which may contribute to abdominal pain after eating or unexplained weight loss. It may also be used to monitor existing arterial disease, or follow-up after surgical intervention.
Why can’t I eat or drink anything before this exam? When you eat, drink, or even chew gum, you swallow air into the stomach and bowel. Excess air in the bowel reduces ultrasound visibility of the mesenteric arteries. Fasting before the exam helps to minimize interference from bowel. In addition, information about the blood flow through the mesenteric arteries is different in a fasting state versus non-fasting. Please let the sonographer know if you have not been fasting prior to this exam.
What happens during the test?
A vascular sonographer will perform the ultrasound exam of your mesenteric arteries. They will ask you to lie on your back on an exam table. You will be asked to raise your shirt halfway up your torso. The sonographer will move a transducer around your abdomen to obtain images. The transducer will have a small amount of gel on the end of it. The gel used during the exam is water-soluble and easily washes off with soap and water. The sonographer may ask you to hold your breath at times during the exam.
You may be asked to drink a fluid, such as Ensure, and wait several minutes before additional images are obtained. This is to see if after you consume something there is a change to the velocity of blood flow in the mesenteric arteries compared to fasting state. A significant increase in the velocity can indicated a stenosis (narrowing of the artery) may be present.
Echocardiography
TRANSTHORACIC ECHOCARDIOGRAM
An echocardiogram uses sound waves to produce images of your heart. This common test allows your doctor to see your heart beating and pumping blood. Your doctor can use the images from an echocardiogram to identify heart disease, irregular rhythms, and more.
Why it’s done: Your doctor may suggest an echocardiogram to check for problems with the valves or chambers of your heart. To check if heart problems are the cause of symptoms such as shortness of breath, palpitations or chest pain. It can also detect congenital heart defects.
STRESS ECHOCARDIOGRAM
A stress echocardiogram, also called an echocardiography stress test or stress echo, is a non-invasive procedure that determines how well your heart and blood vessels are working. During a stress echocardiography, you’ll have ultrasound images of your heart taken before starting exercise on a treadmill while your blood pressure and heart rhythm are monitored. When your heart rate reaches your specific peak heart rate, the technologist will take ultrasound images of your heart immediately after exercise to determine whether your heart muscles are getting enough blood and oxygen while you exercise.
Why it’s done: Your doctor may order a stress echocardiography test if you have chest pain that they think is due to coronary artery disease, which is blockage to the arteries that feed the muscle of the heart. This test also determines how much exercise you can safely tolerate if you’re in cardiac rehabilitation. The test can also tell your doctor how well treatments such as bypass grafting, angioplasty, and anti-anginal or antiarrhythmic medications are working.
